Main content
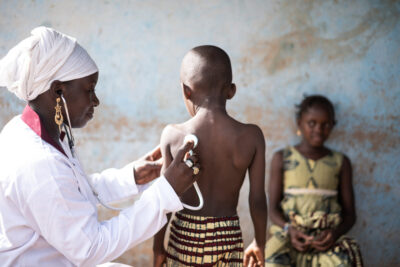
© HelpAge International. Pakistan floods emergency response, Sindh province, Pakistan, 2023
Humanitarian crises caused by conflict, environmental disaster, food insecurity, severe malnutrition, and disease outbreaks are projected to become more complex and protracted over the years and decades to come.[1,2] Since 2020, the frequency, duration and severity of humanitarian crises have multiplied, leaving an estimated 305 million people in need of urgent humanitarian assistance and protection in 2025.[3] By 2050, a fifth of the global population will be over 60, of which 80% will live in LMICs, compared to 60% today.[4] This global demographic shift creates unprecedented challenges in humanitarian crises, which humanitarian actors have been slow to realise.[5] To illustrate, a HelpAge International study into humanitarian financing illustrates the lack of attention to older people’s vulnerabilities and needs. It showed that only 6.5% of humanitarian assistance (392 out of 6,090 projects) was dedicated to meeting the needs of older people.[6]
HelpAge International considers 50 years an appropriate cut-off age for the definition of older persons residing in low-and middle-income countries (LMICs), as it is reflective of changes in their physical capabilities and social roles in LMICs and takes into account lower life expectancies in LMICs.[7]This is supported by the United Nations High Commissioner for Refugees (UNHCR), warning that many challenges associated with ageing will surface earlier (i.e. before 60 years of age) in populations that have experienced trauma, prolonged poor nutrition status, and exposure to disease.[8]
Older adults are a heterogeneous group, and include adults of different ages, gender, ethnicity, sexual orientation, socioeconomic status, displacement status, and disability status. Ageing is not inherently synonymous with vulnerability, yet older people are often framed as a homogenous and vulnerable group.[9,10] This perception neglects the capacities and capabilities of older people who often fulfil pivotal roles in their families and communities in humanitarian crises, including as first responders.[11,12] By drawing on lived experience in disaster- or conflict-prone settings, older people contribute valuable skills, knowledge and social connections, positioning them to meaningfully support emergency preparation, response and recovery when given the opportunity.[13,14]
Ageism as a driver behind exclusion
Reasons for the exclusion of older people in humanitarian crises are multifaceted and include ageism at the institutional, interpersonal and individual level.[15] At the institutional level, barriers and structural challenges often emerge for older people because of ageist attitudes translated into discriminatory laws, policies and priorities, underfunding, and lack of accessibility and affordability of health services. At the interpersonal level, social beliefs and attitudes towards older people play a role in shaping how older people are involved in preparation, response and recovery in humanitarian emergencies. In some cultures, older peoples’ needs and capacities may be discounted, and they may be actively excluded if they are considered less worthy of care and support. Finally, at the individual level, self-directed age discrimination is the result of the internalization of the stigma and marginalization experienced at the institutional and interpersonal levels. When society sees older people as a burden, older people may internalize this view, identify themselves as burdens to their family or society, and act accordingly, for example by neglecting their own health out of fear of becoming a burden on their families.[16] As was apparent during the COVID-19 pandemic, when societies and systems are under pressure, ageism becomes even more pronounced.[17–21] Typically, humanitarian crises put a strain on societies and systems, which in turn can contribute to the strong(er) surfacing of ageism, sexism, racism and other forms of discrimination and oppression.[22–24]
The exclusion of people from the preparation, response, and recovery phases of humanitarian crises on account of age is discriminatory and violates core humanitarian principles. Age-related discrimination violates both the right of older people to receive appropriate, accessible and inclusive humanitarian assistance and the fundamental humanitarian principles of humanity and impartiality.[25]
Meanwhile, humanitarian crises disproportionately affect older people, who may have pre-existing health issues, limited physical functioning, and reduced access to services.[26–29] Their typically higher dependency on social and financial support networks can further increase the risk of adverse health outcomes.[12,27] Older people often have reduced access to safety, health services, clean water, and appropriate food in humanitarian crises, putting them at an increased risk of poor health outcomes including disability, injury, malnutrition, and mental health issues.[30] In addition, older people may have visual and auditory constraints and cognitive deficits, which can create communication challenges.[31]
Non-communicable diseases driving morbidity among older people in humanitarian crises
In humanitarian contexts, chronic disease management is frequently deprioritised in favour of urgent and acute health needs. Outpatient services tend to focus on infectious diseases and acute conditions, while non-communicable disease (NCD) care receives limited attention.[32] A retrospective analysis of routine data from MSF-supported inpatient departments in ten countries, including 149,483 adults, found that older adults were most commonly admitted for NCDs (53%).[33] Compared with younger adults, older adults were more likely to be hospitalised for chronic non-infectious respiratory diseases and acute cerebrovascular or cardiogenic events. Across age groups, women were more likely than men to be admitted for chronic non-infectious respiratory diseases and acute hypertensive crises, while older women were more likely to be admitted for complications of diabetes than older men. These differences may reflect gender disparities in health-seeking behaviours.[34,35] Previous MSF research has shown that delays in seeking care at emergency departments disproportionately affect children and women, largely due to insecurity and limited resources in highly volatile settings.[35] Gender inequalities in access to care may also be influenced by educational gaps, low health literacy, gender roles, and socioeconomic disadvantage.[36,37]
Strengthening age- and gender-responsive NCD care across the continuum of care could reduce avoidable inpatient admissions due to acute NCD exacerbations.[38] This includes greater community participation in health promotion and prevention, more inclusive healthcare design, expanded outreach activities, and strengthened support for community health workers. This includes the provision of palliative and long-term care.[39–41]
Actions to promote age-inclusive healthcare services in humanitarian crises
To work towards age-adapted healthcare services in humanitarian crises, several fundamental challenges need to be addressed including:
- The current absence of a UN convention on the rights of older persons
- The limited uptake and mainstreaming of the minimum standards for age and disability, as well as humanitarian inclusion standards for older people and people with disabilities in policies, guidelines and trainings
- Ageism among humanitarian actors
- Limited availability of earmarked funding for older people
- The lack of a holistic approach to older people’s needs in humanitarian crises
The following recommendations are derived from a broader body of work forming a PhD thesis on the healthcare rights and needs of older people. The thesis comprises a systematic review of existing evidence, the development of a theoretical framework, and empirical analyses of MSF-supported services in humanitarian settings. These analyses examined the health conditions of older people admitted to inpatient departments, the mental health symptoms and precipitating events among those seeking mental health care, and the assault characteristics of older survivors of sexual violence seeking care.
Priority actions to promote more age-inclusive healthcare in humanitarian crises settings:
- Consult older adults and co-create solutions and approaches with them to ensure that their specific needs are not overlooked.
- Ensure commitment among humanitarian actors to ensure age-adapted healthcare services in humanitarian crises through ear-marked funding for the inclusion of older adults in healthcare services and research and accountability mechanisms.
- Prioritise research into urgent research questions related to the healthcare needs of older adults in humanitarian settings, using adaptive research methodologies to ensure inclusion of older adults.
- Strengthen Sex-, Age-, Disability Disaggregated (SADD) data collection, analysis and reporting using five-year cohorts where possible, and 10-year cohorts at a minimum to better understand the health needs of older adults in humanitarian settings.
- Train healthcare staff, health policy makers and health authorities on ageism and age-sensitive healthcare services.
Building on this thesis, we brought together experts, scholars, and practitioners in Utrecht in October 2025 to examine the healthcare rights and needs of older people and to rethink how humanitarian health responses can be more age-inclusive.[42] The next step is to establish a community of practice that unites researchers, operational partners, and national authorities to turn these principles into implementation pathways and priority actions for inclusive humanitarian preparedness and response.
All articles that were part of this thesis can be accessed through the MSF Science Portal: https://scienceportal.msf.org/collections/88
References
- United Nations High Commissioner for Human Rights. Climate resilience and older refugees. OHCHR.
- Aptel C. The Growing Gaps in Global Humanitarian Challenges. 2024.
- OCHA. Global Humanitarian Overview 2025. 2024.
- United Nations Department of Economic and Social Affairs Population Division. World Population Prospects – Population Division. 2022.
- HelpAge International. Ensuring inclusion of older people in initial emergency needs assessments. 2012.
- HelpAge International. Funding for older people in humanitarian crises: reversing continued neglect. 2025.
- HelpAge International. Protection Interventions for Older People in Emergencies. 2013.
- United Nations High Commissioner for Refugees. Older persons – Emergency Handbook. UNHCR.
- Katz AS, Hardy B-J, Firestone M, et al. Vagueness, power and public health: use of ‘vulnerable‘ in public health literature. Crit Public Health. 2020;30:601–11. doi: 10.1080/09581596.2019.1656800
- Munari SC, Wilson AN, Blow NJ, et al. Rethinking the use of ‘vulnerable’. Aust N Z J Public Health. 2021;45:197–9. doi: 10.1111/1753-6405.13098
- Schatz E, Ogunmefun C. Caring and Contributing: The Role of Older Women in Rural South African Multi-generational Households in the HIV/AIDS Era. World Dev. 2007;35:1390–403. doi: 10.1016/j.worlddev.2007.04.004
- Barbelet V, Samuels F, Plank G. The role and vulnerabilities of older people in drought in East Africa: progress, challenges and opportunities for a more inclusive humanitarian response. ODI Think Change. Published Online First: 2 July 2018.
- Shih R, Acosta J, Chen E, et al. Improving disaster resilience among older adults. Rand Health Q. 2018;2.
- HelpAge International. Disaster resilience in an ageing world: how to make policies and programmes inclusive of older people. 2014.
- United Nations High Commissioner for Human Rights. About the human rights of older persons. OHCHR.
- Boetzelaer E van, Kamp J van de, Keating P, et al. Involving older people in the preparedness, response, and recovery phases in humanitarian emergencies: a theoretical framework on ageism, epistemic injustice, and participation. Lancet Healthy Longev. 2024;5:e76–82. doi: 10.1016/S2666-7568(23)00244-1
- Ayalon L. There is nothing new under the sun: ageism and intergenerational tension in the age of the COVID-19 outbreak. Int Psychogeriatr. ;1–4. doi: 10.1017/S1041610220000575
- Derrer‐Merk E, Reyes‐Rodriguez M, Salazar A, et al. Is Protecting Older Adults from COVID‐19 Ageism? A Comparative Cross‐cultural Constructive Grounded Theory from the United Kingdom and Colombia. J Soc Issues. 2022;10.1111/josi.12538. doi: 10.1111/josi.12538
- Fraser S, Lagacé M, Bongué B, et al. Ageism and COVID-19: what does our society’s response say about us? Age Ageing. 2020;afaa097. doi: 10.1093/ageing/afaa097
- Spaccatini F, Giovannelli I, Pacilli MG. “You are stealing our present”: Younger people’s ageism towards older people predicts attitude towards age‐based COVID‐19 restriction measures. J Soc Issues. 2022;10.1111/josi.12537. doi: 10.1111/josi.12537
- Swift HJ, Chasteen AL. Ageism in the time of COVID-19. Group Process Intergroup Relat. 2021;24:246–52. doi: 10.1177/1368430220983452
- Wilbur J, Clemens F, Sweet E, et al. The inclusion of disability within efforts to address menstrual health during humanitarian emergencies: A systematized review. Front Water. 2022;4.
- Rumbach J, Knight K. Sexual and Gender Minorities in Humanitarian Emergencies. In: Roeder LW, Roeder LW, eds. Issues of Gender and Sexual Orientation in Humanitarian Emergencies: Risks and Risk Reduction. Cham 2014:33–74.
- Rohwerder B, Wong S, Pokharel S, et al. Describing adolescents with disabilities’ experiences of COVID-19 and other humanitarian emergencies in low- and middle-income countries: a scoping review. Glob Health Action. 2022;15:2107350. doi: 10.1080/16549716.2022.2107350
- United Nations High Commissioner for Human Rights. Older Persons in Humanitarian Emegencies – The Human Rights Imperative. 2019.
- HelpAge International. Hidden victims of the Syrian crisis: disabled, injured and older refugees – Syrian Arab Republic. 2014. https://reliefweb.int/report/syrian-arab-republic/hidden-victims-syrian-crisis-disabled-injured-and-older-refugees (accessed 3 November 2023)
- HelpAge International. Older people in Africa: a forgotten population. 2008.
- Summers A, Leidman E, Periquito I, et al. Serious psychological distress and disability among older persons living in conflict affected areas in eastern Ukraine: a cluster-randomized cross-sectional household survey. Confl Health. 2019;13. doi: 10.1186/s13031-019-0194-0
- HelpAge International. Health Interventions for Older People in Emergencies. 2012.
- Boetzelaer E van, Rathod L, Keating P, et al. Health needs of older people and age-inclusive health care in humanitarian emergencies in low-income and middle-income countries: a systematic review. Lancet Healthy Longev. 2024;0. doi: 10.1016/j.lanhl.2024.100663
- Bazzi L, Chemali Z. A Conceptual Framework of Displaced Elderly Syrian Refugees in Lebanon: Challenges and Opportunities. Glob J Health Sci. 2016;8:54. doi: 10.5539/gjhs.v8n11p54
- Slama S, Kim H-J, Roglic G, et al. Care of non-communicable diseases in emergencies. The Lancet. 2017;389:326–30. doi: 10.1016/S0140-6736(16)31404-0
- Boetzelaer E van, Keating P, Caleo G, et al. Health conditions of older adults in complex humanitarian settings in low- and middle-income countries: a retrospective analysis of 2019–2025 data from Médecins Sans Frontières-supported inpatient departments. BMJ Glob Health. 2025;10. doi: 10.1136/bmjgh-2024-018667
- Kalindi AM, Houle B, Smyth BM, et al. Gender inequities in women’s access to maternal health care utilisation in Zambia: a qualitative analysis. BMC Pregnancy Childbirth. 2023;23:755. doi: 10.1186/s12884-023-06078-3
- Shaikh BT, Hatcher J. Health seeking behaviour and health service utilization in Pakistan: challenging the policy makers. J Public Health. 2005;27:49–54. doi: 10.1093/pubmed/fdh207
- Hendrickson ZM, Tibbels N, Sidikiba S, et al. ‘I can’t leave everything in the hands of my husband’: Economic constraints and gender roles in care-seeking in post-Ebola Guinea. Glob Public Health. 2022;17:1578–93. doi: 10.1080/17441692.2021.1953107
- Gelaw KA, Atalay YA, Zerefu F, et al. Delays in the decision to seek care and associated factors among mothers who delivered in rural health centers in Wolaita Zone, Southern Ethiopia. Front Glob Womens Health. 2024;4:1236242. doi: 10.3389/fgwh.2023.1236242
- Guzmán IB, Cuesta JG, Trelles M, et al. Delays in arrival and treatment in emergency departments: Women, children and non-trauma consultations the most at risk in humanitarian settings. PLOS ONE. 2019;14:e0213362. doi: 10.1371/journal.pone.0213362
- Rass E, Lokot M, Brown FL, et al. Participation by conflict-affected and forcibly displaced communities in humanitarian healthcare responses: A systematic review. J Migr Health. 2020;1–2:100026. doi: 10.1016/j.jmh.2020.100026
- Asgary R, Garland V, Ro V, et al. A systematic review of effective strategies for chronic disease management in humanitarian settings; opportunities and challenges. Prev Med. 2022;161:107154. doi: 10.1016/j.ypmed.2022.107154
- Thapa R, Zengin A, Thrift AG. Continuum of care approach for managing non-communicable diseases in low- and middle-income countries. J Glob Health. 2020;10:010337. doi: 10.7189/jogh.10.01033742. Van Boetzelaer E. Symposium on ageing in crisis: Advancing the overlooked healthcare rights and needs of older people in humanitarian crises. Speak. Med. Health. 2025. https://speakingofmedicine.plos.org/2025/10/29/symposium-on-ageing-in-crisis-advancing-the-overlooked-healthcare-rights-and-needs-of-older-people-in-humanitarian-crises/ (accessed 13 February 2026)
- Van Boetzelaer E. Symposium on ageing in crisis: Advancing the overlooked healthcare rights and needs of older people in humanitarian crises. Speak. Med. Health. 2025. https://speakingofmedicine.plos.org/2025/10/29/symposium-on-ageing-in-crisis-advancing-the-overlooked-healthcare-rights-and-needs-of-older-people-in-humanitarian-crises/ (accessed 13 February 2026)