Main content
The burden of disease is shifting in many low- and middle-income countries, including Kenya. Whereas the focus was traditionally on infectious diseases, non-communicable diseases such as cancer are now becoming increasingly visible in children as well. In high-income countries such as the Netherlands, approximately 80% of children with cancer survive, whereas in many low- and middle-income countries survival rates remain below 30%. This discrepancy highlights the need for research into the implementation and sustainable scaling up of interventions that improve access to care for children with cancer in such settings. The Princess Máxima Centre for Paediatric Oncology supports this mission through its international department, Máxima International, and its Global Health & Implementation Science research group. Through partnerships with 30 hospitals across low- and middle-income countries, these teams work collaboratively to strengthen paediatric oncology care. Their efforts are closely aligned with the World Health Organization’s Global Initiative for Childhood Cancer, which seeks to increase survival to at least 60% for children with the most common and treatable cancers by 2030.[1]
In this article, we present a research project in Western Kenya that illustrates the implementation of an awareness campaign to improve access to care.
The healthcare system in Kenya
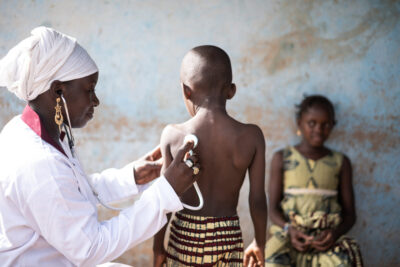
Kenya is a lower-middle-income country with a tiered healthcare system, in which community units, dispensaries, and health centres provide primary healthcare. For many families these clinics are the first point of contact with the healthcare system. In Western Kenya, the Moi Teaching and Referral Hospital (MTRH) serves as the centre for paediatric cancer care. Estimates suggest that 3,000 to 5,000 children in Kenya develop cancer annually, but only 800–900 of them present at the hospital, often at an advanced stage of disease. Most children, therefore, remain undiagnosed. MTRH annually diagnoses approximately 250-300 children with cancer.
Limited access to timely and adequate care for children with cancer is the result of a complex interplay of factors. Symptoms such as persistent fever, weight loss, or swelling are often non-specific and overlap with common childhood illnesses, which can delay referral to specialised care. Specialised paediatric oncology facilities are scarce and concentrated in a few centres, such as MTRH in Eldoret, and Kenyatta National Hospital in Nairobi. For many families, this means long travel distances, high costs, and logistical challenges, which constitute real barriers in the care pathway.
Financial aspects play an important role. Although Kenya has a national health insurance system, coverage for long-term and complex conditions such as cancer is often insufficient. In addition to direct medical costs, expenses for transportation, temporary housing, and daily living place a heavy burden on families. This financial strain affects not only access to care but also the ability to complete treatment.
Cultural factors may also influence timely care-seeking behaviour. Various forms of care, such as traditional or spiritual healing, are part of the care pathway for many families. These forms of care often coexist with formal healthcare, with choices influenced by prior experiences, accessibility, affordability, and trust in the healthcare system.
Together, these factors are not isolated obstacles to access, but an interconnected web that determines when children reach specialised care centres. Understanding this interrelationship is essential to improving access to pediatric cancer care, not only in terms of availability but also in alignment with the context of children and their families.
The awareness programme in Bungoma County
In Bungoma County, a province in Western Kenya, an awareness programme was implemented between 2023 and 2025 in collaboration with local partners (both referral institutes and county governments) to improve recognition of childhood cancer. The programme combined live training sessions for primary healthcare providers with an SMS-based learning programme that enabled healthcare workers to access childhood cancer modules via mobile phone without internet access. In total, 144 training sessions were held, with more than 3,000 healthcare workers trained. The programme also aimed to raise community awareness through a radio campaign and poster distribution, assuming that improved knowledge and awareness among healthcare providers and parents would lead to timely referral to specialised centres. Evaluations show that healthcare providers gained greater knowledge and confidence in identifying childhood cancer through the programme, but this did not automatically translate into an increase in new referrals. Baseline knowledge scores increased significantly (P<0.001) compared with those after the programme. In addition, 181 healthcare providers reported encountering a suspected case after the launch of the programme. However, only 30 newly diagnosed children reached the referral hospital in the prospective follow-up study.[2,3]
What next?
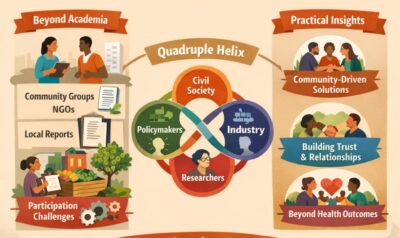
These results underline that knowledge and awareness alone are insufficient. The pathway a patient follows, from primary care provider to a specialised centre, requires a systems approach. It is important that training and awareness programmes are implemented sustainably and that more research is conducted into how referrals can be effectively facilitated, with particular attention to the financial toxicity of this pathway. In addition, community engagement, including local community leaders, traditional healers, and families themselves, is essential to ensure that programmes align with families’ context. Future initiatives will therefore prioritise structured stakeholder mapping and the co-creation of programme designs to enhance contextual relevance, acceptability, and long-term sustainability.
Conclusion
Children with cancer often die not only because of the aggressiveness of their disease, but because barriers within the healthcare system prevent timely diagnosis and treatment. At the same time, there is reason for optimism: the shifting disease burden in many low-income countries, increasing national policy attention to childhood cancer, and growing collaboration between national and international partners are contributing to a rising number of diagnosed and surviving children.
To sustain this progress, we must look beyond individual treatments. Access to care is more than chemotherapy or a hospital bed. It is the entire pathway that a child and their family must navigate each day to reach and to complete treatment, and ultimately achieve a genuine chance of cure.
References
- WHO global childhood cancer initiative [Internet]. [cited 2021 Sep 1]. Available from: https://www.who.int/docs/default-source/documents/health-topics/cancer/who-childhood-cancer-overview-booklet.pdf
- Klootwijk L, Apadet L, El Salih I, Dandis R, Vik T, van de Vijver S, et al. Innovative Training to Improve Childhood Cancer Knowledge Among Primary Health Care Providers: Evaluating a Blended Learning Program in Kenya. JCO Glob Oncol. 2025.
- Klootwijk L, Osamong LA, Kimaiyo S, Vik TA, van de Vijver S, Kaspers G, et al. Barriers to care for newly diagnosed children with cancer from Bungoma County after an awareness campaign: insights from parental interviews and registry data. BMC Cancer. 2025 Nov 19;25(1):1790. doi:10.1186/s12885-025-15098-5