Main content
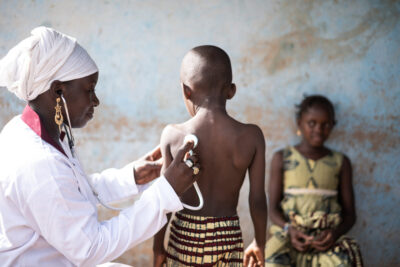
Health inequalities are rarely the result of a single factor. [1] They emerge through interactions between social conditions, economic circumstances, environments and health systems. [2] Interventions developed without meaningful engagement of affected communities often fail to capture this complexity. Co-creation approaches attempt to address this gap by engaging stakeholders directly across planning, conducting, evaluating and reporting research and practice-based initiatives. [2,3] Both in research and practice, co-creation is being applied in several ways to address inequalities.

Tailoring interventions to underserved populations
One common application entails tailoring interventions to underserved populations. [4,5] Programmes working with migrant communities, ethnic minority groups or socially
marginalised populations frequently use participatory methodologies/ co-creation approaches to identify barriers to access, such as language differences, stigma or mistrust
of institutions.[5] Identifying these barriers early allows services and communication strategies to be adapted in ways that are more culturally appropriate and responsive to lived realities.
Improving access through locally informed implementation
In other contexts, co-creation focuses on improving accessibility and implementation. Initiatives in low and middle-income countries and rural settings may engage community
representatives in planning service delivery models or identifying practical solutions to implementation barriers. [4] Interventions can respond more effectively to everyday
constraints that contribute to unequal access to care by incorporating or co-creating local knowledge with relevant stakeholders. [4] For example, efforts to increase diabetes
screening in underserved communities may engage residents and local organisations in identifying barriers such as inconvenient clinic hours, language differences or mistrust of
health services. As a collective, they may adapt how screening is delivered – for instance by offering services in community venues or using culturally appropriate communication. While
the clinical intervention itself does not change, the way it is organised becomes more responsive to local needs.
Participatory approaches in prevention programmes
Prevention programmes also increasingly apply participatory approaches/co-creation [6], although the nature of stakeholder participation and engagement varies depending on the
type of intervention. In programmes focused on behavioural prevention, such as those promoting physical activity, healthy nutrition or mental wellbeing, communities are often engaged in shaping the design and delivery of activities. For example, local residents may help identify barriers to participation, suggest culturally appropriate messaging or co-design activities that fit existing social routines, community spaces or preferred forms of engagement. Such adaptations can increase relevance and uptake, particularly among groups who may not respond to standard public health campaigns.
Participation in clinical prevention programmes
In contrast, clinical prevention programmes, such as vaccination campaigns or screening initiatives, are typically based on established medical protocols and therefore change less fundamentally through participation. However, efforts are being made to better engage stakeholders such as patients, for example through Patient and Public Involvement. [8,9] In
these cases, participatory approaches tend to focus on improving accessibility, communication and trust. Communities may be engaged in tailoring outreach strategies, identifying trusted intermediaries, adapting information materials to different languages or cultural contexts, or determining where and how services are delivered. Rather than altering the intervention itself, participation helps ensure that programmes are implemented in ways that better reflect local needs and address barriers to access.
Co-creation in health system design
Co-creation is not limited to community-facing interventions. [10] Health systems themselves may be redesigned through collaborative processes engaging frontline professionals and service users. [11,12] Such approaches can generate solutions grounded in operational realities rather than implicit theoretical assumptions.
Common patterns across co-creation initiatives
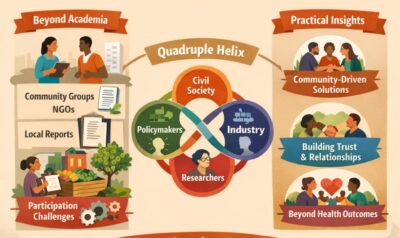
Several patterns emerge across these initiatives. Co-creation frequently extends beyond the health sector, involving links to education, housing or social services. Both stakeholder participation and engagement levels also occur along a continuum, ranging from non-participation to consultation to shared leadership. Evidence suggests that co-creation is inherently multidimensional [13], encompassing multi-stakeholder collaboration, co-learning processes aiming for innovation, contextual knowledge production, shared meaning-making, and open, trustful, inclusive dialogue.
Barriers to participation
However, important challenges remain, as demonstrated in the scoping review evidence. [6] The very conditions that produce health inequalities can also make participation more difficult. Poverty, insecure housing, caring responsibilities and long-standing mistrust of institutions can all limit engagement. Even when participation occurs, stakeholder engagement is often confined to consultation or limited engagement, with relatively few examples of sustained partnership and none reaching full empowerment.
Limits to scaling and transferability
These limitations have implications for both impact and scale. Co-creation initiatives are frequently rooted in local relationships, trusted intermediaries and highly specific contexts. What transfers across settings is rarely the intervention itself, but rather the underlying principles and enabling conditions, including time to build trust, equitable resourcing and engagement across multiple stages of development.
What effective co-creation requires
Co-creation should therefore not be treated as a panacea or a marker of legitimacy. Rather, it requires a structured and intentional approach to collaboration. In practice, this means
clearly defining the roles of different stakeholders, engaging communities at multiple stages of the process – from identifying priorities to shaping implementation and evaluation – and creating mechanisms through which their input can meaningfully influence decisions. It also entails allocating sufficient time and resources for relationship-building, ensuring
transparency about how contributions are used and addressing power imbalances between stakeholders. When these elements are in place, co-creation can strengthen relevance, ownership and sustainability. However, these benefits seem unlikely to emerge when stakeholder participation is limited to one-off consultations or when it is not embedded within broader strategies addressing the social determinants of health.
Read part 1 here
Read part 3 here
References
- Marmot M. Social determinants of health inequalities. The Lancet. 2005 Mar
19;365(9464):1099-104. - Marmot M, Allen J, Bell R, Bloomer E, Goldblatt P. WHO European review of social
determinants of health and the health divide. The Lancet. 2012 Sep
15;380(9846):1011-29. - Messiha K, Chinapaw MJ, Ket HC, An Q, Anand-Kumar V, Longworth GR, Chastin S,
Altenburg TM. Systematic review of contemporary theories used for co-creation, co-
design and co-production in public health. Journal of Public Health. 2023
Sep;45(3):723-37. - Leask CF, Sandlund M, Skelton DA, Altenburg TM, Cardon G, Chinapaw MJ, De
Bourdeaudhuij I, Verloigne M, Chastin SF, GrandStand, Safe Step and Teenage
Girls on the Move Research Groups. Framework, principles and recommendations
for utilising participatory methodologies in the co-creation and evaluation of public
health interventions. Research Involvement and Engagement. 2019 Jan 9;5(1):2. - Longworth GR, Erikowa-Orighoye O, Anieto EM, Agnello DM, Zapata-Restrepo JR,
Masquillier C, Giné-Garriga M. Conducting co-creation for public health in low and
middle-income countries: a systematic review and key informant perspectives on
implementation barriers and facilitators. Globalization and Health. 2024 Jan
17;20(1):9. - Messiha K, Thomas N, Brayne C, Agnello DM, Delfmann LR, Giné-Garriga M, Lippke
S, Downey J. Grey literature scoping review: a synthesis of the application of
participatory methodologies in underrepresented groups at an elevated risk of
dementia. BMC Medical Research Methodology. 2025 May 3;25(1):122. - Catley A, Alders RG, Wood JL. Participatory epidemiology: approaches, methods,
experiences. The Veterinary Journal. 2012 Feb 1;191(2):151-60. - Bagley HJ, Short H, Harman NL, Hickey HR, Gamble CL, Woolfall K, Young B,
Williamson PR. A patient and public involvement (PPI) toolkit for meaningful and
flexible involvement in clinical trials – a work in progress. Research Involvement and
Engagement. 2016 Apr 27;2(1):15. - Elliott RS, Taylor E, Ainsworth J, Preston J, Smith EM. Improving communication of
the concept of ‘treat-to target’ in childhood lupus: a public and patient (PPI)
engagement project involving children and young people. BMC Rheumatology. 2022
Oct 15;6(1):69. - Fusco F, Marsilio M, Guglielmetti C. Co-creation in healthcare: framing the outcomes
and their determinants. Journal of Service Management. 2023 Dec 18;34(6):1-26. - Elg M, Engström J, Witell L, Poksinska B. Co‐creation and learning in health‐care
service development. Journal of Service Management. 2012 Jun 22;23(3):328-43. - Anand-Kumar V, Schreier M, Bakshi N, Messiha K, Longworth GR, An Q, Angello
DM, Chastin S, Lippke S. Facilitators and challenges of co-creating digital public
health interventions: A Health CASCADE multi-case exploratory study. Public health.
2025 Oct 1;247:105847. - Messiha K, Altenburg TM, Giné-Garriga M, Chastin S, Chinapaw MJ. Enriching the
existing knowledge about co-creation: identifying dimensions of co-creation using
explicit theory in various research fields. Minerva. 2025 Feb 17:1-24.